BY MIKA YOKOTA
Introduction
The Spring Festival on January 25, 2020 has become an unexpected and unforgettable memory for the people of China. On December 31, 2019, Wuhan Municipal Health Commission authorities reported multiple pneumonia cases of unknown etiology in Wuhan, Hubei Province. A series of events that followed disallowed the country to celebrate the renowned annual festival. On January 1st, the Huanan Seafood Wholesale Market in Wuhan linked to the first four reported cases closed. The city went into lockdown on the 23rd. Then, COVID-19 was proven capable of human-to-human transmission. With countries such as Italy, Iran, and Japan reporting surging cases early in the year, the World Health Organization (WHO) declared COVID-19 a pandemic on March 11, 2020. Quarantine and social distancing measures were then implemented as safety guidelines. With the world in an emergency health crisis, not only is the physical aspect of health a number one priority, but the mental aspect of health also remains in need of attention. Constant isolation and the deprivation of human interaction have caused trouble for many across the world. The pandemic has undoubtedly impacted people’s psychosocial wellbeing, with emphasis on sleep, anxiety, and suicide.
Background
Mental Aspect
Seeing the constantly rising cases, anxiety creeps in and tickles the unsettled mind. COVID-19 has transformed hugs and kisses into weapons. Not visiting grandparents became an act of love, and money has lost its power. Quarantine has devastated the world economy and the mental wellbeing of many. Extensive periods of isolation and social distancing may give rise to concerning mental health issues.
The Science Behind Sleep, Anxiety, and Suicide
There are four stages of sleep, separated into Rapid Eye Movement (REM) and non-REM sleep. The first non-REM stage is called N1. It is the stage between sleep and wakefulness, where the brain starts to produce theta waves. Hypnagogic hallucinations may occur along with hypnic jerks. People are harder to awaken during N2. More theta waves are produced along with sleep spindles, which are bursts of rhythmic brain activity that help inhibit some cognitive processes; the k-complexes produced suppress cortisol arousal and keep people asleep and aid memory consolidation. N3 is a deeper stage of sleep where the person is “dead to the world”. The Electroencephalogram (EEG) will show a much slower frequency with high amplitude signals – delta waves. This is the stage where people walk or talk in their sleep. REM is the stage associated with dreaming. The EEG resembles wake time, but the body is in a state of sleep paralysis to prevent the person acting out their dreams. Despite having four stages, sleep is a 90-minute cycle with N3 returning to N2 before entering REM: N1->N2->N3->N2->REM.
We need sleep for various reasons, including recuperation, mental function, and growth. Yet, COVID-19 has heightened levels of stress and anxiety, disrupting our natural rest pattern. Cortisol, our stress hormone, should be at low levels when entering sleep; the level gradually rises as we wake up. But, stress can cause the curve to be reversed. High cortisol levels at bedtime hinders the ability to fall asleep. Glucocorticoid receptors will be activated, leading to elevated cortisol releasing hormone, which decreases short wave sleep. Light sleep is increased, and wakes during the night occur more often, which leads to more anxiety and stress regarding falling asleep. This vicious cycle impedes the replenishment of the circadian rhythm, and blood sugar levels may also plunge into chaos and spike during the evening.
And, above mentioned emotional instability caused by objective isolation or perceived loneliness both contribute to suicidal ideation. This pandemic may cause increased suicidal rates during and even after the crisis.
Discussion
Healthcare Workers
A survey was sent out through Chinese social media by health departments in Shenzhen to examine the public’s mental health burden. Results demonstrated that the healthcare worker group – doctors, nurses, healthcare administrators – showed the most significant mental strain due to the pandemic. Their group also reported the highest rate of poor sleep quality (23.6 percent), evaluated with the Pittsburgh Sleep Quality Index (PSQI), with a P-value less than 0.001, allowing us to reject the null hypothesis that ‘there is no relationship between COVID-19 and sleep quality in health workers’. The higher number for health workers comes as no surprise as 16-hour shifts and exhaustion from the frontline fighting deprive them of proper recuperation, raising the risks of chronic stress, distress, and anxiety.
Additionally, the hours dedicated to evaluating the pandemic situation were revealed to contribute to stress levels. Most nurses spend over three hours thinking about the pandemic per day due to the intensity of their contact with COVID patients and their need to assist with the daily living of the ill. Coupled with the wearing of humid, air trapping personal protective equipment and diapers for their whole shift, the nurses have completed their duty in exchange for their wellbeing. A female nurse from Hubei Province that joined the COVID ward on February 4th commented that she found it extremely tough to carry out normal processes such as venipuncture due to the thick layer of gloves; reading medicine labels has also become hard of a task since the goggles blur up. “I am very anxious and irritable, because I have so much work to do but I can’t see well.” she said.
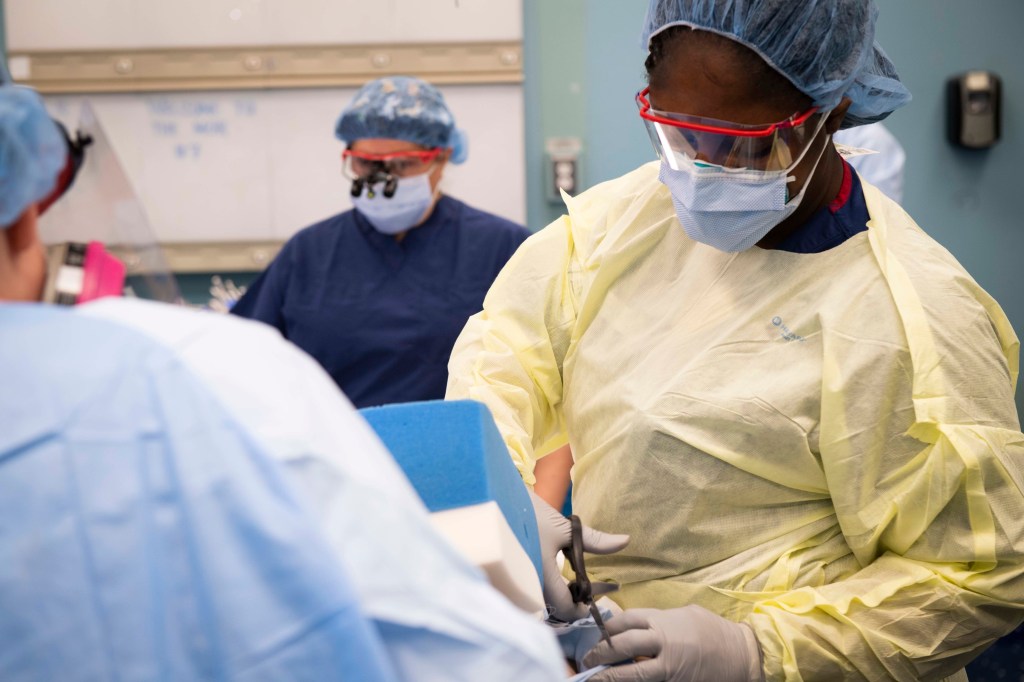
Doctors and physicians must continuously review the government’s COVID-19 guidelines and policies with colleagues and decide on how to proceed. Along with the health administrators organizing them all into the COVID-19 ward, they have to juggle all the problems while simultaneously acquiring new skills with speed. In an interview conducted on February 13, 2020, a physician in Hubei province, specialized in oncology, said: “I have to treat patients who are not in my specialty…it is an unknown disease and everyone feels powerless.” Some teams even included healthcare workers from other provinces; this diverse and multidisciplinary team had to find ways to collaborate and communicate effectively and quickly.
Moreover, a study showed that 34 percent of healthcare workers experienced insomnia. In Wuhan versus not in Wuhan, frontline versus second line, and secondary hospital versus tertiary hospital, medical workers in the former were more susceptible to anxiety and insomnia. Unusual sleep patterns are a stand-alone risk factor for suicidal thoughts, attempts, and death. A 37-year-old Japanese health worker who managed isolated returnees from Wuhan, China was reported to have committed suicide.
Teachers and Students
With strict guidelines regarding school reopening after the winter holiday, most schools opted for online learning. The extensive period lacking physical interaction has challenged adolescent and young adult’s mental strength. Although remaining home appears as a scarce opportunity to spend time with family, the limitations may outweigh the benefits. Physical education classes have been canceled, or the possibilities restricted. Sporting facilities are closed and remain such until governments authorize the openings. Exercise has long been considered a potential remedy for sleep disorders such as insomnia and a vital maintainer of sleep patterns. Improved fitness from aerobic endurance activities and hour-long acute exercises have been proven to be most beneficial.
Moreover, with students managing their upcoming examinations and applications, it is not easy with teachers spread across the globe; sleep adjustments must be made. A faculty of Sports Science indicated that earlier wakes were required to ensure no students were falling behind. A ninth-year student commented that communication barriers developed with peers and teachers in other countries; another exclaimed that her “social life has been disturbed!”. If the sudden transition to remote operations was not frustrating enough, students faced the reality of exam cancellation. Final examinations have been canceled by many organizations, including the International Baccalaureate Organisation (IBDP), Cambridge International Education (CIE), Pearson, and College Board, etc. This has left the student panicking, fearing postponement and grade prediction complications.
Enterprise and Institution Workers
Unemployment in the U.S. is rising towards unprecedented levels since the Great Depression. And, the uncertainty drifting through the news is contributing to anxiety levels. Data released by the International Labour Organisation on March 18, 2020, declared a decline of 24.7 million jobs and 5.3 million jobs, as the high and low scenario, respectively. Suicide is also closely linked with unemployment, as the lack of secure income creates emotional and physical vulnerabilities.
Conclusion
The focus of the news on the transmission of the virus within various countries in the world has diverted attention from the equally demanding psychological aspect of the pandemic that may translate into long-term ramifications. A holistic response should contain physiological and psychosocial information and resources for the affected and the general population. Researchers should continue their work on COVID-19’s effect on several components of mental health, identifying additional measures to address pandemic related psychosocial issues while maintaining consistent effort to counteract the physical spread of the virus.
——————————
References:
- Statement from WHO. (2020, April 27). Archived: WHO Timeline – COVID-19. World Health Organization. https://www.who.int/news-room/detail/27-04-2020-who-timeline—covid-19.
- Khan Academy. Sleep stages and circadian rhythms (video). Khan Academy. https://www.khanacademy.org/test-prep/mcat/processing-the-environment/sleep-and-consciousness/v/sleep-stages-and-circadian-rhythms.
- Stress Hormones: The 4 Major Stress Hormones. Its Psychology. (2017, July 15). https://itspsychology.com/stress-hormones/.
- Sher, L. (2020). The impact of the COVID-19 pandemic on suicide rates. QJM: An International Journal of Medicine. https://doi.org/10.1093/qjmed/hcaa202
- Huang, Y., & Zhao, N. (2020). Generalized anxiety disorder, depressive symptoms and sleep quality during COVID-19 epidemic in China: a web-based cross-sectional survey. Elsevier Psychiatry Research , 288. https://doi.org/10.1101/2020.02.19.20025395
- Huang, Y., & Zhao, N. (2020). Generalized anxiety disorder, depressive symptoms and sleep quality during COVID-19 epidemic in China: a web-based cross-sectional survey. Elsevier Psychiatry Research , 288. https://doi.org/10.1101/2020.02.19.20025395
- Liu, Q., Luo, D., Haase, J. E., Guo, Q., Wang, X. Q., Liu, S., … Yang, B. X. (2020). The experiences of health-care providers during the COVID-19 crisis in China: a qualitative study. The Lancet Global Health, 8(6). https://doi.org/10.1016/s2214-109x(20)30204-7
- Liu, Q., Luo, D., Haase, J. E., Guo, Q., Wang, X. Q., Liu, S., … Yang, B. X. (2020). The experiences of health-care providers during the COVID-19 crisis in China: a qualitative study. The Lancet Global Health, 8(6). https://doi.org/10.1016/s2214-109x(20)30204-7
- Buysse, D. J. (2013). Insomnia. Jama, 309(7), 706. https://doi.org/10.1001/jama.2013.193
- Lai, J., Ma, S., Wang, Y., Cai, Z., Hu, J., Wei, N., … Hu, S. (2020). Factors Associated With Mental Health Outcomes Among Health Care Workers Exposed to Coronavirus Disease 2019. JAMA Network Open, 3(3). https://doi.org/10.1001/jamanetworkopen.2020.3976
- Sher, L. (2020). COVID-19, anxiety, sleep disturbances and suicide. Sleep Medicine, 70, 124. https://doi.org/10.1016/j.sleep.2020.04.019
- Huang, Y., & Zhao, N. (2020). Generalized anxiety disorder, depressive symptoms and sleep quality during COVID-19 epidemic in China: a web-based cross-sectional survey. Elsevier Psychiatry Research , 288. https://doi.org/10.1101/2020.02.19.20025395
- Daniel, S. J. (2020). Education and the COVID-19 pandemic. Prospects. https://doi.org/10.1007/s11125-020-09464-3

