BY KELLY FARLEY
One third of the world’s population is infected with a latent form of it.1 Without treatment, 50% of those with the active form will die.2 We have a cure. And yet every day 5,000 people die of tuberculosis (TB).2
Background
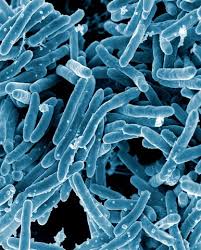
TB is an infectious disease caused by the bacterium Mycobacterium tuberculosis.3 A patient can have either dormant (known as “latent TB”) or active TB. Latent TB affects 2 billion people,4 while active TB affects 10 million.5 In latent TB, the body’s immune system is strong enough to keep the bacteria in check; there are no symptoms, and, unlike active TB, the disease cannot be transmitted to others.3 An estimated 5-10% of latent TB infections progress into active TB, if the patient is immunocompromised and the bacteria may multiply uncontrollably.6 Active TB is transmitted when a person infected with active TB coughs or talks, spreading the bacteria into the air.7 Contrary to the stigma surrounding the disease, TB is not extremely contagious; infection requires prolonged exposures in enclosed environments, such as households, workplaces, prisons, or schools.8 TB primarily affects the lungs, though it can spread to the kidneys, spine, and brain.3 This can lead to symptoms such as a persistent cough, coughing up blood or sputum, chest pain, fatigue, and fever.9
History
In the Western world, TB is thought of as a disease of the past. In the United States, it is; the overall TB case rate is 2.9 cases per 100,000 persons,10 meaning that the percentage of people presenting with TB is less than 0.003%. Yet, just 200 years ago, TB – known as “consumption” at the time – was widespread in Western Europe and North America.11 In 1900 through 1980, the rate of TB in Western Europe and the United States decreased to 1/100th of the previous level, mainly because of improvements in hygiene and living conditions.11 As the average number of people living in one room declined from eight to one or two, the amount of TB cases also declined.12
As HIV spread in the 1980’s, TB levels again increased. Those infected with HIV are 30% more likely to develop active TB because of their weakened immune systems.4 Initially, the medical community largely ignored the problem – which is why Dr. Lloyd Friedman, a clinical professor of medicine at the Yale School of Medicine and a pulmonary critical care specialist at Yale-New Haven Hospital, was drawn to studying it. In his words, TB has always been the “underdog.”13 From 1984 through 1992, Dr. Friedman followed the incidence of HIV and TB in substance abusers in New York and found that “the rates of tuberculosis, AIDS, and death are extremely high.”14 However, the outbreak was quickly controlled because of the developed health infrastructure in New York City.13
This was not the case in developing, low-income countries. In 1993, the World Health Organization (WHO) officially declared TB a global emergency as rates skyrocketed alongside those of HIV.4 In 2014, the WHO committed to ending TB by 2030.15 In 2018, it is still a global emergency without much progress towards ending it by 2030. As Dr. Ted Cohen, an associate professor of epidemiology and an infectious disease epidemiologist at the Yale School of Public Health, explained, “Tuberculosis is a disease of poverty.”16 In developing countries, living conditions are more compact and enable the disease to spread much faster.16 In addition, people in developing countries are more susceptible to developing active TB because of the weakened immune systems that accompany malnutrition.16 In South Africa, one of the countries with the highest burden of TB, 80% of the population is infected with latent TB and 0.8% develop active TB.17 The incidence of TB in South Africa is 250 times that of the United States.1 The risk of disease is highest in infants, lowest in children until 10 years of age, and then rises during adolescence and remains high.1 The disease is two times more common prevalent in men than women because men tend to work outside of the home and are thus exposed to more bacteria.18
Diagnosis in the Community Setting
In the opinion of Dr. Luke Davis, a pulmonary critical care physician at Yale-New Haven Hospital and an associate professor of epidemiology and medicine at the Yale School of Public Health, TB research should prioritize the four million undiagnosed cases; diagnosis is important and also easiest to fix.18 In a 2017 study of TB diagnosis in the community setting (i.e. outside of clinics), Dr. Davis analyzed the dropout rates associated with the four steps of TB diagnosis: 1) scheduled home visits; 2) initiated house visits; 3) TB screening; 4) further TB evaluation.19 Ultimately, there is a 5% probability that a person completes all 4 steps of the pathway, meaning that many patients go undiagnosed.19 The biggest dropout rates were steps two and four. 50% of patients made it through step two.19 In the other 50% of cases, the patient is no longer located at the same address for a variety of reasons – perhaps because he/she had to move elsewhere so that family could care for him/her, because he/she was exiled from the home because of the disease, or because he/she had to give up the home after losing a job due to TB.19 Only 20% of patients make it through step four, potentially because of the cost and difficulty associated with going to the clinic for further TB evaluation.19 Knowing where the issues with diagnosis stem from enables interventions to improve diagnosis, such as home visits followed by a phone call instead of a clinic visit, community education about TB, minimizing the stigma associated with TB, and increasing trust between health workers and patients.
Treatment and Antibiotic Resistance
Currently, latent TB can be treated with a 9-month regimen of one or two antibiotics that kills actively replicating mycobacteria.20 Active TB is treated with a 6-month combination of four antibiotics to avoid antibiotic resistance.20 Nevertheless, since antibiotics are the primary method used for treating TB, antibiotic resistance still poses a problem for its treatment, especially since patients do not always finish their course of antibiotics.21 Multidrug-Resistance TB is resistant to the most common treatments and accounts for about 5% of all TB cases.1 Extensively Drug-Resistant TB is rarer but particularly worrisome because it is also resistant to two more drugs.21
Because typically only one antibiotic is used for preventive TB therapy, there have been concern about whether preventive therapy should be used if it may increase the likelihood of antibiotic resistance. However, Dr. Cohen’s 2016 mathematical modeling of TB suggests that the benefits of preventative therapy outweigh the risk of antibiotic resistance, particularly in countries like Botswana where the rates of TB have been declining.22 In general, TB rates worldwide have been declining as HIV treatment improves, implying that preventive therapy should be more widely used.

Credit: Torange.Biz
A more significant cause of TB antibiotic resistance is that patients stop their antibiotics before the course of treatment has finished. TB treatment requires 6 months of antibiotic treatment because TB is not always actively dividing.18 But, like with other diseases, patients tend to stop taking medications when they feel better.18 Patient education efforts primarily revolve around the disease itself and do not include information relevant to the patient’s daily life, such as how to remember to take it daily, where to get refills, and how to cope with stigma from the community.18
The cultural stigma surrounding TB is strong enough to dissuade patients from traveling to the clinic to be diagnosed and more than strong enough to dissuade patients from continuing to take their medication for months on end. In developing countries, TB is associated with unsanitary conditions and poverty.12 Since TB is transmitted through the air, there is also a misconception that TB is highly contagious, which further adds to the stigma.18 Dr. Davis remembers how the brother of a clinician in Uganda hid his pills instead of taking them and ultimately died of TB.18
New Developments
Dr. Friedman believes that our hope for decreasing TB lies in vaccines, which have prevented many infectious diseases, past and present.13 The current Bacillus Calmette-Guérin vaccine is primarily used in infants who have not yet been exposed to TB.1 98 years since its invention, we finally have hope for a TB vaccine that could also be given to patients with latent TB. On September 27, 2018, the results of the phase 2b trial of the M72/As01E candidate vaccine was published and showed 54% efficiency.23 According to Dr. Friedman, this new vaccine is efficient because, “One, you only have it give it once and it works. Two, it works on latent disease. Three, it will work for drug resistant organisms.”13 The ability to target latent disease is key, since 80% of new cases are derived from the latently infected pool, and would allow us to drop the rate of TB much faster than current methods.13 Nevertheless, this vaccine lacks funding. Because it will be primarily used in low-income countries, pharmaceutical companies are hesitant to invest in its clinical trials.13 Currently, the vaccination lacks the funding to progress to a phase 3 trial.13
On September 26, 2018, the United Nations (UN) held its first high-level meeting on TB, bringing much needed attention to the disease and beginning to remove the years of stigma.24 The meeting’s theme was “United to end tuberculosis: an urgent global response to a global epidemic.”24 The meeting identified TB as an urgent matter affecting all countries. But some have questioned whether the goals established by the meeting will ever actually be achieved. The International Union Against Tuberculosis and Lung Disease criticizes the lack of accountability established by the UN.25 Only poor nations are affected by TB; only rich nations have the power to fix it.

Credit: WHO
The Future
The global community should clearly invest in TB treatment because of the 5,000 people this curable disease kills every day. As Dr. Davis explains, these 5,000 people represent “the most marginalized people in every community.”18 These are the people living in poverty, commonly with HIV, in countries that are all too frequently overlooked.
There are also health and even economic incentives to intervention. In Dr. Cohen’s words, “Tuberculosis does not respect borders.”16 As an infectious disease, TB can spread globally; if the deaths in other countries are not a pressing enough reason for intervention, then countries may consider their own risk of TB infection. Additionally, treatment prevents people from fleeing, leading to social and economic stability in a country and worldwide.18
When asked if we will be able to meet the WHO’s goal to end TB by 2030, all three Yale researchers/professors interviewed immediately responded, “No.” Right now, curing TB is not the priority. It is controlling TB – quickly. As Dr. Cohen put it, “The bar is low for saving lives.”16 So many people are affected by TB that any intervention at all will save so many lives. There is work to be done and a difference to be made.
Kelly Farley is a sophomore in Morse College studying Chemistry and Statistics & Data Science. She may be contacted at kelly.farley@yale.edu.
——————————
References:
- Pai, M., Behr, M., Dowdy, D., Dheda, K., Davigangahi, M., Boehme, C., Ginsberg, A., … Raviglione, Mario. (2016, Oct.). Tuberculosis. Nature Reviews Disease Primers, 2, 1-23.
- Herriman, R. (2017). World TB Day 2017: Responsible for 5000 deaths daily. Outbreak News Today. Retrieved from http://outbreaknewstoday.com/world-tb-day-2017-responsible-5000-deaths-daily-37626/.
- Tuberculosis. (2018). Centers for Disease Control and Prevention. Retrieved from https://www.cdc.gov/tb/?404;https://www.cdc.gov:443/tb/topic/basics/default.htm.
- McIntosh, J. (2017). All you need to know about tuberculosis. Medical News Today. Retrieved from https://www.medicalnewstoday.com/articles/8856.php.
- Tuberculosis: Data and statistics. (2017). Centers for Disease Control and Prevention. Retrieved from https://www.cdc.gov/tb/statistics/default.htm.
- TB risk factors. (2016). Centers for Disease Control and Prevention. Retrieved from https://www.cdc.gov/tb/topic/basics/risk.htm.
- How TB spreads. (2016). Centers for Disease Control and Prevention. Retrieved from https://www.cdc.gov/tb/topic/basics/howtbspreads.htm.
- Tuberculosis. (n.d.). American Lung Association. Retrieved from https://www.lung.org/lung-health-and-diseases/lung-disease-lookup/tuberculosis/.
- Tuberculosis: Latent TB infection and TB disease. (2016). Centers for Disease Control and Prevention. Retrieved from https://www.cdc.gov/tb/topic/basics/tbinfectiondisease.htm.
- Burden of TB in the United States. (2017). Centers for Disease Control and Prevention. Retrieved from https://www.cdc.gov/features/burden-tb-us/index.html.
- Lafrance, A. (2016). The danger of ignoring tuberculosis. The Atlantic. Retrieved from https://www.theatlantic.com/health/archive/2016/08/tuberculosis-doomsday-scenario/494108/.
- McKie, R. (2018). Scientists warn of global crisis over failure to tackle tuberculosis. The Guardian. Retrieved from https://www.theguardian.com/society/2018/sep/15/global-tuberculosis-crisis-scientists-warn-united-nations-summit.
- Friedman, Lloyd. (2018, Oct. 11). Phone interview.
- Friedman, L., Williams, M., Singh, T., & Frieden, T. (1996, March). Tuberculosis, AIDS, and death among substance abusers on welfare in New York City. The New England Journal of Medicine, 334, 828-833.
- The end TB strategy. (n.d.) World Health Organization. Retrieved from https://www.who.int/tb/strategy/en/.
- Cohen, Theodore. (2018, Oct. 12). Personal interview.
- TB statistics for South Africa: National & provincial. (2016). Retrieved from https://www.tbfacts.org/tb-statistics-south-africa/.
- Davis, Luke. (2018, Oct. 5). Personal interview.
- Armstrong-Hough, M., Turimumahoro, P., Meyer, A., Ochom, E., Babirye, D., Ayakaka, I., … & Davis, J. (2017, Nov.). PLOS ONE, 1-13.
- Fox, G., Dobler, C., Marais, B., & Denholm, J. (2017, Mar.). Preventative therapy for latent tuberculosis infection—the promise and the challenges. International Journal of Infectious Diseases, 56, 68-76.
- Drug-resistant TB. (2017). Centers for Disease Control and Prevention. Retrieved from https://www.cdc.gov/tb/topic/drtb/default.htm.
- Kunkel, A., Crawford, F., Shepherd, J., & Cohen, T. (2016). Benefits of continuous isoniazid preventive therapy may outweigh resistance risks in a declining tuberculosis/HIV coepidemic. AIDS, 13(30), 2715-2723.
- Van Der Meeren, O., Hatherill, M., Nduba, V., Wilkinson, R., Muyoyeta, M., Van Brakel, E., … & Tait, D. (2018, Sept.). Phase 2b controlled trial of M72/AS01E vaccine to prevent tuberculosis. The New England Journal of Medicine, 379, 1621-1634.
- UN General Assembly high-level meeting on ending TB. (2018). World Health Organization. Retrieved from http://www.who.int/tb/features_archive/UNGA_HLM_ending_TB/en/.25. United Nations high-level meeting on tuberculosis. (n.d.) International Union Against Tuberculosis and Lung Disease. Retrieved from https://www.theunion.org/un-high-level-meeting-on-tb.
