BY KRISTI WHARTON
Tommy Hill played many different roles in his life: a son, a boyfriend, a brother, a mentor. All of this ended July 10th, when he was found dead in his apartment after overdosing on heroin. For about a year, Tommy managed to stay clean, going to meetings and even mentoring others struggling with the problem of addiction, a problem he knew all too well. One of those mentees was his friend Scotty Hamblin. The two had grown up together playing as children and eventually, battling heroin addiction together. Tommy became Scotty’s sponsor as he made his was through a sober living program and counseling sessions on what could have been his road to recovery. Instead, Tommy’s death lead Scotty to relapse, falling back into a heroin-dependent life.1
On that day in July, though, Tommy became one of the 18 people who would overdose over the course of the following week in Cincinnati alone. Throughout America, one person dies every 16 minutes from heroin and synthetic opiate use, making it the leading cause of death for Americans under the age of 50. The approach to resolving this issue, called the war on drugs, tries to prevent addiction by interdicting against drug use and reducing illegal drug trade via police intervention. This method has not worked, however, because it does not approach addiction as the disease that it is. 2 The opioid epidemic, which in October 2017 was declared a public health emergency by President Trump, will not improve until it is understood that people suffering from addiction need access to treatment and rehabilitation, not incarceration.
The United States has grappled with the issue of opioid abuse since before the turn of the 20th century. During the Civil War, injured soldiers were often treated with morphine and became addicted to the powerful opioid. In 1898, heroin production started on the commercial scale and became known as a “wonder drug” whose effects could be intensified if administered through injection. During this time period, people knew that these drugs were effective painkillers and utilized them as such. They did not become aware of their addictive nature until the 1920s. Soon after these findings, doctors refrained from using these forms of treatment, and heroin was made illegal in 1924. 3

Source: whitehouse.gov
Learning from past mistakes, by the 1970s, doctors were wary of prescribing highly addictive opiates to patients. This changed when articles were published with the argument that opiates could safely be prescribed to those suffering from chronic pain, as long as the patient did not have a history of addiction. By the ‘90s, people were less concerned about a repeat of the 1970s heroin epidemic, and there was a newfound emphasis on pain management. 3
One of the doctors who published an article arguing that there was minimal risk of addiction when using opiates explained that he was trying to make primary care physicians feel more comfortable about opioids. But, in the process of de-stigmatization, they often overlooked evidence. He said on the matter, “Clearly if I had an inkling of what I know now then, I wouldn’t have spoken in the way that I spoke. It was clearly the wrong thing to do.”3
Opioid addiction rates have continued to grow over the years, and as a result, the number of overdoses has also increased. The CDC Director, Tim Frieden, wrote in the New England Journal of Medicine, “We know of no other medication routinely used for a nonfatal condition that kills patients so frequently.” He also explained that recent studies have shown that one out of every 550 patients who started using opioids died of opioid related causes an average of 2.6 years after their first prescription. 3 These numbers only apply to those prescribed the opioids, but there are also users abusing heroin and other non-prescribed synthetic opiates.
When heroin or other opiates are injected into the body, they travel through the bloodstream up to the brain. They are converted into morphine by enzymes in the body and then find opiate specific receptors in the brain to bind to. Now they are able to decrease pain perception and increase dopamine levels, which can trigger sensations of euphoria. Dopamine levels can rise to almost ten times their normal levels when heroin is in the body. There are endogenous opioids produced by the body, such as endorphins, that bind to the opiate receptors; however, the sensations felt from heroin are greatly amplified compared to the naturally occurring endorphins.6
After regular exposure to opioids as well as the sustained, elevated dopamine levels, the body begins to build up a tolerance to the drugs. Pain signaling sensitivity is intensified, and pain thresholds are decreased. These changes can take effect as quickly as after just one use. The increased sensitivity of the pain signaling pathways causes them to become overactive. As a result, users feel as though they need the drug to feel normal. 6
In places like Huntington, West Virginia and Cincinnati, Ohio, the epidemic is impacting everyone, from users to first responders and even to newborns. In regions like these, it is not uncommon for one week to consist of 180 overdoses, 18 heroin or synthetic opiate related deaths, 200 heroin users in jail, and 15 babies born with heroin related medical problems. Parents are losing children, and children are losing parents. 1
Patsy Uebel works as a nurse at the Cincinnati Children’s Hospital Medical Center, treating babies suffering from neonatal abstinence syndrome. This condition occurs when the infant’s mothers are addiction to heroin or use while they are pregnant. The symptoms can include seizures, tremors, or other common withdrawal symptoms. She saw one patient, Elliana, when she was eight months old. When asked about Elliana’s development, specifically her ability to hold things, her mother, Stephanie, proudly explains that she picks things up, throws them on the ground them, and then looks at them and laughs. Stephanie has used heroin and other opiates for years, but quit when she found out she was pregnant. She explains that she just wants to be able to have a normal life with her daughter. Patsy tells Stephanie that Elliana looks great, and asks to see them back in a few months. Ten days later, Stephanie is found dead from a heroin overdose. 1
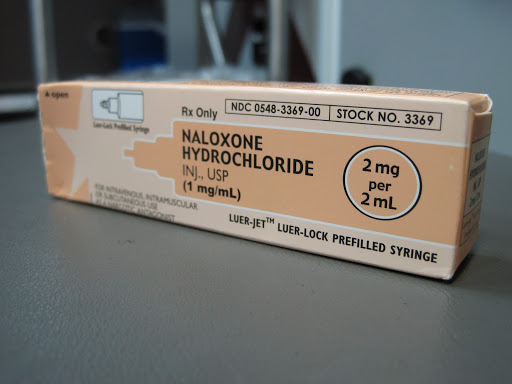
First responders in these parts of the US see overdoses like this everyday. If found quickly enough, people can sometimes be saved, even after their heart stops, by a drug called Naloxone. Naloxone is able to reverse the effects opiates by binding to opiate receptors and reversing the effects of the drug. Naloxone can be injected or administered through a nasal spray, making it easy to give to first responders or even to the public to reduce the number of deaths from overdose.4
Jan Rader, the Deputy Chief of the Huntington Fire Department firmly believes all first responders should have Naloxone with them treat overdoses, and she works hard to ensure all first responders in her county have supplies of Naloxone with them at all times. Some people believe that Naloxone enables addicts; there is less consequence associated with overdose if it can be reversed. Rader explains that this is not the case. Naloxone isn’t enabling, because it actually induces withdrawal symptoms. She says that often times people get mad after receiving a treatment of Naloxone because they feel “dope sick”. She goes to explain, “The only qualification for getting into the long term recovery is you have to be alive. I don’t care if I save somebody 50 times. That’s 50 chances to get into long term recovery. People do go into long term recovery and they do become productive citizens, tax paying citizens.” Additionally, people who have been through the recovery process often go on to help and mentor others going through similar experiences. 4
These long term recovery programs are the alternative to the war on drugs. While the war on drugs results in addicts going to jail, the long term recovery programs offer help and support for those trying to reform.
While some people maintain the opinion that policemen are not doctors and should not carry Naloxone, many officers have taken on a new role in their communities. They help individuals suffering from addiction get the treatment they need, and they administer the opioid reversal drug when necessary.
One day in Piatt Park in Ohio a bike cop saw a man passed out on a bench. He called for paramedics and administered a dose of Naloxone he had with him. When the paramedics arrived, they gave the man another dose of Naloxone, successfully reversing the effects of the drug the man had overdosed on. While this is an example of the benefits of cops being equipped with Naloxone, it is unfortunately not the beginning of the man’s road to recovery. Although encouraged to go to the hospital, the man rose from the bench and walked away, ignoring the advice. This is not the desired response to the incident, but as Jan Rader explained, saving the lives is worth it. Even if they have to do it again, that is one more chance for him to go into recovery. 4
Currently, Attorney General Jeff Sessions is still advocating to cut treatment funding, ultimately reviving the war on drugs. What little funding there is goes towards the consequences of untreated addiction and isn’t being spent on treatment and prevention, which would fight the problem at the source. Putting people in prison increases prison population, and criminal justice and health care costs, and fails to address the disease. Additionally, a stigma has been created around the issue, creating yet another barrier to face when trying to handle this problem. At the 30th DARE training conference in July 2017, Sessions stated, “We have to create a cultural climate that is hostile to drug abuse.” 2,5
President Trump made promises to aid communities who are afflicted by this epidemic. He proposed providing those suffering from addiction with treatment rather than jail time. Although, he has put much of his time and energy into attempting to dismantle the ACA and Medicaid: programs that previously provided millions of addicts with proper addiction care and health care services. He also has spent time on a “tough on crime approach,” regardless of the fact that more people are dying from overdoses than are from homicide. 2
Source: Opiate Support Group
In the hardest hit regions, member of the community are coming up with ways to help wherever they can. In Covington, near Cincinnati, a woman named Scarlett Hudson works with a non-profit called the Women of Alabaster Ministries, Inc. Their mission is to assist women who are caught in human trafficking and grappling with addiction. She drives the women to appointments, and twice a week she does outreach ministry where the women can get food, shower, a nap, clothes and see a nurse once a week. Hudson also drives around handing out bags with food, toothpaste, shampoo, and various other toiletries the women may need. Hudson is affectionately known around the area as “Momma Scarlett,” and the women know they can call her if they need help. Hudson explains that the most important part of the work she does is not judging the women for the difficulties they are facing. 1
The growing epidemic must be fought tactfully, recognizing addiction as a disease, and treating it as such. More funding must be invested in addiction prevention and treatment strategies. The goal should be not to break down, but to build up a health care system that offers individuals with addiction access to the help they require. The issue is growing and spreading, and affecting a vast population. In Cincinnati, a crowd of people to gathered at the Sheriff’s office to receive pamphlets and door hangers with information about addiction and treatment. The county’s judge official asked them if they had been affected by the heroin crisis. To those who didn’t raise their hands he said, “You are touched by it. You just don’t know it yet.” 1,2
——————————
References:
- Heroin in Cincinnati: This is what an epidemic looks like. (n.d.). Retrieved February 01, 2018, from https://www.cincinnati.com/pages/interactives/seven-days-of-heroin-epidemic-cincinnati/
- Will Declaring the Opioid Epidemic a National Emergency Lead to a Public Health Approach or a Return to the War on Drugs? (2017, October 17). Retrieved February 01, 2018, from https://www.centeronaddiction.org/the-buzz-blog/will-declaring-opioid-epidemic-national-emergency-lead-public-health-approach-or?gclid=EAIaIQobChMI6ZGzrYv02AIV1xeBCh3bxAb4EAAYAyAAEgKaIPD_BwE
- Moghe, S. (2016, October 14). Opioids: From ‘wonder drug’ to abuse epidemic. Retrieved February 01, 2018, from https://www.cnn.com/2016/05/12/health/opioid-addiction-history/index.html
- Elaine Mcmillion. (2017, September 12). Heroin(e). Retrieved January 20, 2018, from https://www.netflix.com/watch/80192445?trackId=13752289&tctx=0%2C0%2Cb30ba3a0e018a04daa23c404b992b97fa3d99fe8%3A2ee4e69709f4752f941bce54dede6102f16c5881
- Attorney General Jeff Sessions Delivers Remarks at the 30th DARE Training Conference. (2017, July 11). Retrieved February 01, 2018, from https://www.justice.gov/opa/speech/attorney-general-jeff-sessions-delivers-remarks-30th-dare-training-conference
- Safe Landing Recovery. (n.d.). Retrieved February 02, 2018, from https://heroin.net/heroin-effects/heroin-effects-sub-page-1/heroin-effects-on-the-brain/
