BY GRACIE JIN
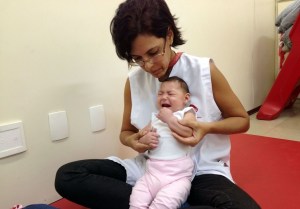
18-year-old Ianka Barbosa cradles her baby daughter, Sophia, in her parents’ tiny brick house in northeast Brazil. She was 7 months pregnant when she learned that Sophia had microcephaly, the incurable condition causing atypically small heads, severe birth defects, and intellectual disability, which doctors blamed on the Zika virus. Before Sophia was even born, her father had left. “I think, for him, it was my fault the baby has microcephaly,” Barbosa said to journalists from New York Magazine. “When I most needed his help, he left me.”1
Barbosa is not alone. On February 1, 2016, the World Health Organization officially declared Zika a public health emergency of international concern.2 At the time, Zika transmission had already been reported in 23 countries, with 4,180 suspected cases of microcephaly in Brazil. In July 2016, 93.4 million people were at risk of Zika infection in Latin America and the Caribbean, 1.7 million of which were childbearing women.3
Since Zika currently has no vaccine or treatments beyond symptom alleviation, health officials have focused instead on prevention campaigns. In January 2016, many Latin American health ministers advised that women postpone pregnancy for six months to two years due to the Zika outbreak.4 However, these recommendations placed the whole burden of disease on women, blindly ignoring the controversial fact that 56% of pregnancies in the region are unintended. Zeid Ra’ad Al Hussein, UN Commissioner for Human Rights, explained the gender-biased response: “the advice of some governments to women to delay getting pregnant ignores the reality that many women and girls simply cannot exercise control over whether, when, or under what circumstances they become pregnant, especially in an environment where sexual violence is so common”.5 The Zika epidemic is unveiling tragic failings of reproductive health policies in Latin America. Due to the poor quality of sex education, lack of access to contraception, and high prevalence of rape, many women in Latin America have little control over their reproductive lives.
Hidden behind the staggering numbers and horrific photographs are stories of young mothers like Barbosa. Governments cannot wait for science to find a cure when Zika is crippling generations of mothers and children. To propose effective steps toward reproductive rights reform, Latin American health leaders must first examine maternal and child health as key to global development, then understand the factors exacerbating the problem: socioeconomic inequality and religious conservatism. Finally, governments must adopt culturally-sensitive policies around termination of pregnancy, education, and support services for women affected by Zika.
Maternal and child health ranks near the top of global health priorities and indicates a country’s standard of living. Every year, more than half a million women—99% of whom live in developing countries—die in pregnancy and childbirth due to preventable reasons. In Latin America, high maternal mortality rates often affect the poor, rural, and indigenous. 55% of women in Nicaragua give birth at home, 65% are illiterate, and adolescents account for almost one-third of maternal deaths. Maternal-related health issues are the most common reason for public hospital admission in Nicaragua (29%), followed by pneumonia and diarrhea.6 These statistics place into context the lack of reproductive health knowledge, resources, and support in Latin America that render women powerless to fight against the arrival of an epidemic as explosive as Zika.
Latin America and the Caribbean are the most unequal regions in the world. The Zika epidemic reflects this egregious socioeconomic inequality. Zika is concentrated among poor, young, women of color from underdeveloped regions, who live in crowded neighborhoods exposed to mosquito breeding grounds, and who have the least access to reproductive health care. In addition to poor sanitation and substandard housing, the irregular water supply forces families to store water at home and spread the mosquito vector.7 In Managua, the capital city of Nicaragua, most of the over 150 informal settlements lack water service.
The World Health Organization recognizes that “the burden of Zika falls on the poor”.8 Policies that neglect reproductive rights increase gender inequality by placing overwhelming financial burden on women. These strains begin with detection and diagnosis: “to identify if you have had Zika, the cost in private labs is close to 1000 reals (just over $250),” explains Brazilian activist and former Global Fund for Women board chair Jacqueline Pitanguy; “the majority of women cannot afford it.”4 In addition to costs incurred during pregnancy, women in many Latin American cultures are responsible for child care. The New York Times reports accounts of many mothers of infants with Zika-related disabilities who have been abandoned by their partners. In the impoverished Campina Grande, ground zero of the Zika epidemic, psychologist Jacqueline Loureiro works at a specialized microcephaly clinic to help mothers cope with stress and trauma. Only 10 out of the 41 women she counsels receive adequate support from their partners.9 “At first many of the women say they have a partner, but as you get to know them better you realize the father is never around and the baby and mother have effectively been abandoned,” Loureiro said. After the Bishop of São Paulo stated that women should take the care of babies with microcephaly as their mission, these mothers faced extreme loneliness, social stigma, and the effects of being stripped of their financial autonomy due to abandonment.6 With no ability to generate an income and little public health assistance, for women who already face an intergenerational cycle of poverty, “their childbearing dreams turn into nightmares because of the Zika virus.”10
While inequality is a root cause of the Zika epidemic, some risk factors of infection that can be addressed more readily include poor sex education and a lack of access to reproductive health services. Among the 18 Zika-active countries, the estimated Contraception Prevalence Rate (CPR) in 2015 was as low as 37.8% (Haiti) or 44.8% (Guyana).3 This reproductive health knowledge gap is often linked to cultural and religious conservatism. The WHO estimates that 22% of women across Latin America want to delay or prevent pregnancy but do not have access to birth control, are misinformed, or are not educated about contraception due to strong conservative dogmatism. This lack of education has led to high rates of teenage pregnancy in Latin America: 38% of girls and women get pregnant before the age of 20.4
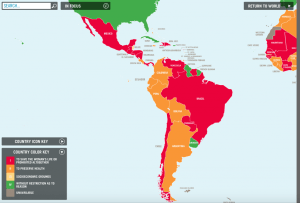
While the landmark decision of Roe v. Wade is often taken granted for in the United States, many countries affected by Zika have some of the strictest termination of pregnancy (TOP) laws on the planet. Abortion is allowed in Guatemala, Haiti, Honduras, Paraguay, Suriname, and Venezuela only to save a mother’s life, whereas in the Dominican Republic, El Salvador and Nicaragua, TOP is illegal in all situations.11 Voluntary interruption of pregnancy faces constant threats of retrocession, as politicians debate stiffening laws to give jail terms of 4.5 years to women who abort fetuses with microcephaly.
Why are abortion laws so strict, especially in Central America? Spanish and Portuguese colonial law, which followed Catholicism, left a blueprint for the post-independence 1810 Napoleonic codes in Latin America. Instead of equating abortion with homicide and a death sentence like under Canon Law, the civil codes in Latin America criminalized abortion with imprisonment.12 Few modern politicians would consider publicly supporting the legalization of abortion, in fear of losing support of their conservative constituents and the Church. Nicaraguan President Daniel Ortega has strongly supported his country’s total ban on abortion. Strict abortion laws refused to budge even when the Zika epidemic struck. Recently, Pope Francis suggested that contraceptives may be used to prevent the spread of Zika virus despite the Catholic Church’s ban on most forms of birth control; in the same statement, he called abortion “an absolute evil” and a crime like “what the Mafia does”. These sentiments resonate deeply with the Brazilian people, who are 65% Catholic. According to a poll conducted in February 2016, 58% of Brazil’s population did not support the right to abortion for women infected with Zika.10
While abortion is morally and culturally controversial, the undeniable fact is that the current system criminalizes poor women. To access abortions, women either have to have enough funds to pay for illegal procedures or fly out of the country. Approximately 850,000 Brazilian women have illegal abortions annually, and about 200,000 were hospitalized in 2013 because of complications.6 In Latin America, the Guttmacher Institute estimates that the total number of abortions rose to 4.4 million, 95% of them in unsafe conditions. One doctor in El Salvador described a case where a woman put caustic soda inside her vagina. Instead of ending her pregnancy, she was so badly burned she had to have a caesarean.13
These horror stories highlight a desperate need for reform in reproductive health policies across Latin America. In Brazil, abortion is the fourth leading cause of maternal mortality, demonstrating that the current legislation saves neither embryos nor mothers. In El Salvador, some women face up to 40 years in jail on abortion charges. These disproportionately include poor women, single mothers, and rape victims. Some were not aware of their pregnancy and miscarried; others suffered complications near the end of their pregnancy and could not seek help in time. One international effort to tackle this criminalization debacle, “Las 17”, demanded the release of seventeen women imprisoned due to their miscarriages. Since the campaign launched in April 2014, two women have been released. The other 15 are still in prison.11
Governments must take action as they wait for scientists to find a cure for Zika. First, realistically adapt abortion policies, taking into account the culture of each community. Simply changing the law is not enough, however, and schools must educate girls to increase knowledge about reproductive rights and access to contraceptives. Third, provide financial and social support for women whose livelihoods are threatened by Zika. Last and more broadly, incorporate human rights issues such as gender equality into the global health approach in order to better respond to future epidemics and allocate resources to where unmet need is highest.
Firstly, women should have the right to make fully informed decisions about their pregnancies. The Office of the United Nations High Commissioner for Human Rights recommended an “urgent revision” of Brazil’s reproductive rights legislation so that all women, especially those in fear of carrying a fetus with microcephaly, may have the right to choose whether to proceed with or interrupt the pregnancy, protecting their physical and emotional integrity without “moral condemnation and criminalization”.7 Just as abortion sparks controversy in the United States, climates around the legalization of abortion vary across Latin America. Monica Arango from the nonprofit Center for Reproductive Rights explains that while South America is making advances in women’s rights, Central America is a place where “it is dangerous to be a woman of reproductive age”. When Uruguay decriminalized abortion in 2012, it became only the second country to do so in Latin America, after Cuba. 13
Universal legalization of abortion may be an unrealistic goal, but maximizing reproductive rights reform will require joint effort across all sectors including the government, the courts, and the nonprofit community. On August 24, 2016, the National Association of Public Defenders petitioned for Brazil’s Supreme Court to allow termination of pregnancy in the case of women under “great mental suffering” from contracting the Zika virus. Joaquim Neto, president of the association, qualifies that “abortion would only occur in very exceptional cases,” and that the mental suffering would have to be verified by psychologists. “Abortion is not the main goal of the petition, but it is impossible to talk about Zika without addressing abortion”.11
While Neto gives voice to the silent and vulnerable in the sphere of public policy, nonprofit organizations have also stepped up. In countries where women have no universal access to safe abortions, the nonprofit Women on Web (WoW) provides online telemedicine to help terminate pregnancy including mifepristone and misoprostol. Since the Zika alert issued by the Pan American Health Organization, WoW received statistically significant increases of between 36% and 108% in requests for abortion. From November 2015 to March 2016 in Brazil, the number of requests doubled as a total of 1,210 women requested abortions while only 581.7 requests were expected (P<0.001).14 This overwhelming flood of requests reveals not only the need for safe abortions for the 56% of women in Latin America who did not intend their pregnancies, but also the government’s unfulfilled responsibilities. Ignoring these cries for help will put the whole weight of a public health crisis on individual women, depriving them of their dignity and financial autonomy.
While reproductive health policy change is crucial for sustainable reform, legislation is ineffective without implementation through awareness and education. The situation in Colombia serves as an example of this gap. Although Colombia has one of the loosest abortion laws in Latin America, which allows women to terminate their pregnancies under circumstances including rape, birth defects, or risks to the mother’s physical and mental health, the Global Fund for Women reports that legal abortions in Colombia remain extremely rare because women have difficulty accessing doctors who will perform abortions.4
Another gap in women’s health education was unveiled by a British Medical Journal study on the prevalence of sexually transmitted diseases, HIV, and cervical neoplasia, which involved 1,185 women who attended health clinics in Nicaragua. Almost one out of five women had an STI, and 1 out of 13 had a precancerous lesion of the cervix. While only 30.4% of the women visited the clinic for STI-related reasons, 77% reported symptoms after probing.15 These numbers show a gaping lack of knowledge in STI prevention, screening, and treatment in Nicaragua. The government must take responsibility to improve the current state of women’s health education.
Key strategies to combat this lack of access include starting sex education in public middle schools and increasing wider community knowledge about family planning and contraceptives. While much research is underway to understand the Zika virus and develop treatments for Congenital Zika Syndrome, few studies have examined the impact of Zika on family planning. Understanding the causes of Zika-related neurological disorders will help women make informed decisions about their pregnancies, but in the short term, initiatives to help women achieve their basic health needs are crucial.
As a human right, comprehensive reproductive health information should be provided to all women. Education efforts to reach women affected by Zika, who are already vulnerable due to socioeconomic inequality, must be strengthened. In addition to incorporating sex ed into middle school health curricula, possible methods of education outreach include informational displays at community centers, pamphlets delivered to health clinics, posters at grocery stores, speakers at public spaces, and various events catering to specific cultures. Clinics should adopt programs that equip nurses and doctors with the skills to respond to Zika; schools could train students to be peer health educators; government agencies and nonprofits could organize sex education and vaccination campaigns at rural clinics and urban hospitals.
Furthermore, several organizations currently work to advance reproductive rights and women’s health education in Zika-affected regions. The Institute for Bioethics in Brazil demands accessible and affordable contraception. The Catholics for the Right to Decide network aims to soften extremist religious rhetoric in Latin America through reproductive health education. The SOS Corpo Instituto Feminista para a Democracia, directed by Silvia Camurça, is leading a national movement for sexual and reproductive rights in Brazil. These organizations coalesce to help women realize their rights, advocate for them, and connect to services for safe motherhood.
The positive effects of education are well-established globally. Studies in Africa and Latin America show that women’s education lowers their risk of HIV and other sexually transmitted infections, increasing their comfort and ability to discuss HIV with a partner.16 These advances made by education can and should be replicated for Zika-related reproductive health issues.
Policy and education emphasize prevention, but governmental response to the Zika epidemic must not neglect social and financial support for women who already gave birth to children with congenital Zika syndrome. First, public health clinics must offer mental health services in addition to Zika testing. The stresses of women who are pregnant, infected with Zika, and uncertain about their pregnancies can be emotionally traumatizing. To better understand the emotional toll Zika takes on women, researchers evaluated mothers at a public clinic in Sergipe, Brazil, between November 2015 to June 2016. They compared data on anxiety, depression, and quality of life between two groups: one of which was comprised of nine mothers whose infants have microcephaly, and the other 20 mothers who had healthy newborns. The results confirmed the researchers’ fears. ZIKV-related microcephaly is significantly associated with high levels of anxiety and low scores in the psychological domain of the WHO quality of life questionnaire (P = .006) for mothers 24 hours after childbirth.17 To combat anxiety and increase self-esteem in mothers of children with Zika congenital infection, multidisciplinary counseling and psychoeducational intervention programs should be implemented.
Second, financial support is crucial to preserving long-term autonomy of women and families impacted by Zika. The current system of social assistance in Brazil limits financial benefits for families with babies with microcephaly to three years, but public lawyer Neto counters that “the disability of these children is permanent”.18 Sadly, the women in need are already among the poorest and most vulnerable; 66% of the babies with Zika-related birth defects have been born in Brazil’s Northeast, one of the least developed regions. For these women, financial assistance should be coupled with education programs to help them become fiscally independent. Instead of leaving already marginalized women and children behind to suffer the worst repercussions of Zika, the state must lighten their burden through social and financial support.
The Zika epidemic echoes a broader problem in the current global health system: a lack of focus on gender and other diverse human rights issues during emergency response. Making women-specific recommendations to avoid pregnancy, without considering the structural gender inequality that deprive women of control over their reproductive lives, is a grave mistake. To bridge this disconnect between international health officials and those most victimized by the epidemic, the voices of women must be heard. To address the root causes of maternal mortality, the Zika epidemic, or any other women’s health issue, governments must view gender as a social and economic determinant of health.
Barbosa and her boyfriend got back together three months after Sophia was born. The psychologist for mothers at the microcephaly clinic had encouraged their reunion. Although Sophia is still too young for doctors to assess her neurological and physical delays, Barbosa worked hard to teach her to speak and was incredibly proud to hear Sophia say “Mama” for the first time. Although an X-ray in Barbosa’s apartment shows irreversible calcification in Sophia’s brain, her mother has not given up. Barbosa takes Sophia to physical therapy sessions twice a week at the hospital’s microcephaly unit, which also offers donated formula and diapers. Although Barbosa’s family has a hard time getting by, she decided to help other women in similar situations by organizing an online fundraiser called Amor Maior, “Bigger Love”, which brought in 40,000 reals (approximately $11,000) in its first year. Barbosa distributed 1,200 reals (about $345) to 25 mothers.1
On November 18, 2016, the WHO removed the status of Zika as a global health emergency. However, for the women whose babies are affected by Zika, the disease remains painfully close to home. Just as much remains unknown about the workings of the Zika virus, much uncertainty awaits Sophia’s future. “While Sophia is making progress, there are things she will never be able to do,” Barbosa laments, “we really don’t know what her future holds.” But instead of being hesitant like she used to, Barbosa says that she is “not afraid to ask for what [she] needs for [her] children.”1 Barbosa’s story of abandonment and tragedy has transformed into a tale of empowerment and hope. For the millions of women affected by Zika in Latin America, reproductive health education and comprehensive support are key to helping them escape poverty, realize their rights, and live lives of dignity. This is not just a fight for public health, but also one for women’s rights and social justice.
Gracie Jin is a freshman in Berkeley College interested in studying neurobiology, global affairs, and medical anthropology. She can be contacted at grace.jin@yale.edu.
__________
References:
- Bauza, P. (2016). Life After Zika: What It’s Like to Raise a Baby With Microcephaly. New York Magazine. Retrieved from http://nymag.com/thecut/2016/12/after-zika-raising-baby-with-html
- Zika declared public health emergency in wake of explosive spread, possible link to birth defects (2016). The Nation’s Health. Retrieved from http://thenationshealth.aphapublications.org/site/misc/ZikaVirusNations020216.xhtml.
- Roa, M. (2016). Zika virus outbreak: reproductive health and rights in Latin America. The Lancet,387(10021), 843.
- News Update: Is Zika a tipping point in the fight for reproductive rights in Latin America? (2016). Global Fund for Women. Retrieved from https://www.globalfundforwomen.org/is-zika-a-tipping-point-for-reproductive-rights-in-latin-america/
- Child and Maternal Health Issues in Nicaragua. (2016). Foundation for Sustainable Development. Retrieved from http://www.fsdinternational.org/country/nicaragua/healthissues
- Diniz, D. (2016). The Zika Virus and Brazilian Women’s Right to Choose. New York Times. Retrieved from https://www.nytimes.com/2016/02/08/opinion/the-zika-virus-and-brazilian-womens-right-to-choose.html
- Moron, A. F. (2016). Zika virus outbreak and reproductive rights. BJOG: An International Journal of Obstetrics & Gynaecology,124(4), 549-549.
- Vélez, A. C., & Diniz, S. G. (2016). Inequality, Zika epidemics, and the lack of reproductive rights in Latin America. Reproductive Health Matters, 24(48), 57-61.
- Eisenhammer, S. (2016). Reuters. Brazil’s mothers left to raise microcephaly babies alone. Retrieved from https://www.yahoo.com/news/brazils-mothers-left-raise-microcephaly-babies-alone-165156957.html?ref=gs
- Collucci, C. (2016). Brazilian attorneys demand abortion rights for women infected with Zika. British Medical Journal, I4657.
- Anderson, C. F. (2016). Reproductive Inequalities. NACLA Report on the Americas, 48(1), 15-17.
- Diniz, D. (2016). Zika virus, women and ethics. Developing World Bioethics, 16(2), 62-63.
- Watson, K. (2015). How inequality limits reproductive rights in Latin America. BBC World News. Retrieved from http://www.bbc.com/news/world-latin-america-32703342
- Aiken, A. R., Scott, J. G., Gomperts, R., Trussell, J., Worrell, M., & Aiken, C. E. (2016). Requests for Abortion in Latin America Related to Concern about Zika Virus Exposure. New England Journal of Medicine, 375(4), 396-398.
- Claeys, P. (2002). Prevalence and risk factors of sexually transmitted infections and cervical neoplasia in women’s health clinics in Nicaragua. Sexually Transmitted Infections, 78(3), 204-207.
- Haynes, D. (2016). Tackling Zika Requires Tackling Inequality. Huffington Post. Retrieved from http://www.huffingtonpost.com/douglas-haynes/tackling-zika-requires-ta_b_9376294.html
- Oliveira, S. J. G. D. S., Melo, E. S., Reinheimer, D. M., Gurgel, R. Q., Santos, V. S., & Martins-Filho, P. R. (2016). Anxiety, depression, and quality of life in mothers of newborns with microcephaly and presumed congenital Zika virus infection. Archives of Women’s Mental Health, 19(6), 1149-1151.