BY DIKSHA BRAHMBHATT

“So, where exactly is Swaziland?” is a question I became all too familiar with as I shared stories of my experiences during a Yale Summer Session class, “Visual Approaches to Global Health.” Honestly, I was poorly equipped to answer that question before I decided to fly to South Africa and Swaziland, a neighboring landlocked monarchy of just over 1.4 million people.1 During our two weeks in Johannesburg and four weeks in Swaziland, we witnessed the striking aftermath of the Apartheid, still alive and well, even outside of the Apartheid museum. In the coal mines that dot the landscape just outside of Johannesburg, the oppression of black people continues. Men from all over southern Africa flock to the mines with hopes of earning a living for their families back home. In doing so, they assume a life dominated by over-crowded quarters, a high risk of HIV, and a lack of health care. Mr. Mkoko, a friend of our professor, lives in rural Swaziland but moved away to work in a South African coal mine. When he returned, he brought home both HIV/AIDS and multidrug-resistant tuberculosis. We traveled to his village of Kashoba, where he is now an HIV community educator and an empowering figure promoting treatment awareness.
Over a quarter of Swazis live with HIV, and the resulting high death rate has lowered the life expectancy to 49 years, with a third of the population currently below age 14.2 My global health courses only vaguely familiarized me with these statistics. While they are crucial for assessing the need for resources and action, they only paint half of the picture. I did not realize just how meager my understanding of the complexity of global health issues was until I took this course, which allowed me to study abroad with Professor Jonathan Smith, a filmmaker and lecturer in Epidemiology of Microbial Diseases and Global Health at the Yale University School of Public Health. When I see the number 3,500, which approximates the annual deaths attributed to HIV/AIDS in Swaziland, I now force myself to look beyond the number to the meaning that lies within.3 That number does not just describe the quantity of people killed by a vicious viral disease. That number represents a host of social, political, health, and economic issues that plague Swaziland. Although AIDS is a preventable, treatable disease, it burdens one’s life for a lifetime. That number hides the fact that antiretroviral therapy only became accessible in Swaziland in 2003, even though the therapy became available the United States as early as 1996.4 That number hides the loss of productivity caused by the disproportionate prevalence among those aged 15-24, particularly women. That number hides gender-based violence and a deep-running current of stigma associated with AIDS that has debilitated efforts to create change.
My Story
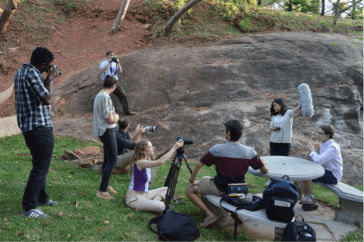
My interest in global health issues flourished after taking an introductory course with Professor Richard Skolnik. This course helped me realize the power of prevention, education, and treatment beyond the offices of physicians. With the encouragement and advice of mentors and peers, I made my way to southern Africa. I expected to go on adventures and visit “cool” places, all while enhancing my understanding of health policy, data, and social welfare. By the end of six weeks, I realized that I had severely underestimated the learning curve that came with staying in a foreign country, especially one suffering from such a significant lack of medical care. Our professor lectured and gave us assignments, but he emphasized that these were only supplementary to what the local people taught us: the local hotel staff, the people we interviewed for the documentary we made as a class, and the Swazis with whom we formed friendships. They all taught me that behind the data lie stories that need to be heard.
Their Stories
Meet Mr. Vusi Matsebula. He was the second person in Swaziland to publicly declare his HIV status in 1996, after three years of feeling like he was alone in his fight. His HIV counselor, who was assigned to him at the onset of his diagnosis in the early 90s, provided him with tremendous support and introduced him to others who were experiencing the same feelings of isolation, confusion and shame. Yet, he found it most difficult to convey his status to his mother. Though, when she found out through Vusi’s sister, his mom immediately opened up her arms to him. Her solidarity and affection gave him the strength to become an activist and create the Swaziland AIDS Support Organization, a national organization that provides education and counseling to families affected by HIV in even the most rural areas. He truly believes that his group provides a welcoming community and teaches families to be sympathetic and supportive. It gives people the motivation to not only get tested, but also to seek treatment, even in the face of possible social repercussions.
Meet Sibonginkhosi Mawela. He is 20 years old and volunteers at an NGO-funded HIV clinic in the heart of the capital city of Mbabane. His mother works at the hotel we stayed at, and encourages his volunteer work even though he is not remunerated. He is HIV-negative. We asked him why he is forgoing the more traditional paths to a secure income, instead offering his youth, energy and time to educating his peers about protected sex and younger children about health and loving their bodies. For Sibonginkhosi, his activism started when he witnessed his HIV-positive friend refuse to go to a clinic for medication out of fear of being publicly recognized. Sibonginkhosi realized that this stigma caused more damage than the virus itself. As a young person, he feels an obligation to work to ameliorate an issue that directly impacts his life. He distributes condoms discreetly at bars because he knows these alcohol-fueled environments are breeding grounds for high-risk behavior. Even though he does not currently have the funds to pursue higher education, he is a valuable asset in the struggle toward a better understanding of HIV prevention and treatment as it pertains to his own community.
Our Story
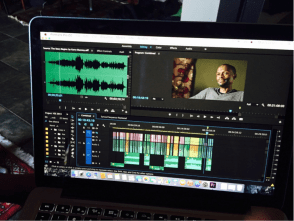
Data can never tell the full story; I have found that human lives and personal interactions with those whom data represent can help contextualize numbers on a page. My global health courses meant more to me after I became friends with families like the Matsebulas and the Mawelas. I saw how the burden of disease trickled into all aspects of their lives. Vusi thought he would never be a father because he was afraid of passing HIV to his child, though ultimately his daughter was born HIV-negative. Sibonginkhosi fears that stigma from others seeing him as HIV-positive will limit his future marriage prospects.
Our class actively sought compelling narratives and learned to piece together casual conversations, information from class, discussions from a multinational conference on Mine Workers’ Compensations and TB, and the informal and formal interviews we conducted. As Professor Jonathan Smith explains, we used film to translate an epidemic to an emotion. We hoped to produce a tangible product that would convey not only the severity of HIV prevalence and stigma, but also to depict hope and inspiration for our primary target audience, Swazi youth. Our documentary, a product of hours upon hours of story-chasing, filming, and editing, portrayed a story of social and institutional discrimination against those living with HIV, as well as current local and national efforts to combat it. More importantly, however, we tried to portray the strength of the human spirit within people who persevered despite daunting statistics. We wanted our work to be a call-to-action for Swazi youth, and an inspiration for them to change the dialogue, or lack thereof, surrounding the stigma that affects someone they know, if not themselves.
If you would like to read the blog our class produced, visit http://yss2015.epidemictoemotion.org/.
For more information on Jonathan Smith’s projects, visit http://epidemictoemotion.org/.
Diksha Brahmbhatt is a sophomore in Berkeley College. Diksha is an Anthropology major from Florida. She can be contacted at diksha.brahmbhatt@yale.edu.
________
Works Cited:
1) Central Intelligence Agency. (2015). Swaziland. CIA: The World Factbook. Retrieved from https://www.cia.gov/library/publications/the-world-factbook/geos/wz.html.
2) HIV & AIDS in Swaziland. (2012). Avert: Averting HIV & AIDS. Retrieved from http://www.avert.org/hiv-aids-swaziland.htm.
3) Swaziland HIV & AIDS Estimates. (2014). UNAIDS. Retrieved from http://www.unaids.org/en/regionscountries/countries/swaziland.
4) Bartlett, J. (February 2006). Ten Years of HAART: Foundations for the Future. Medscape. Retrieved from http://www.medscape.org/viewarticle/523119.
